The two major things to keep in mind
When managing low-back pain in an active person, consider these structural and neurological components.
First, address the structural component, beginning from the ground up.
In most cases, the feet, knees and hips follow common patterns. Generally, the most significant distortion in the lower extremity is observed in a typical low–back pain patient during the mid-stance phase.
Mid-stance, a phase during which the heel and toes maintain contact with a surface, usually presents the foot in a state of maximum pronation. Concurrently, the distal femur and proximal tibia surfaces are internally rotated alongside a corresponding internal rotation of the femur heads.
The feet: Managing hyperpronation for better posture
Hyperpronation is one of the most commonly encountered conditions affecting the feet. A very predictable pattern occurs in the navicular, cuboid, cuneiforms, metatarsal heads, talus and calcaneus. Hyperpronation often appears bilaterally and asymmetrically, contributing to pelvic tilt, frequently observed in patients with low–back pain. Bringing the feet into equilibrium is essential to create a balanced and stable posture.
On average, we take 7,000–10,000 steps per day; each heel strike while walking carries 2.5 times our body weight. Over time, the plantar fascia and many other bone-to-bone ligaments, like the spring ligament, may elastically deform. This deformation can cause the foot to become less stable.
Therefore, adjusting and stabilizing the foot is primary in creating the balanced pedal foundation needed to treat low–back pain.
My vision for ideal foot support during the functional gait cycle includes the following:
- Permitting the optimal or standard range of foot motion.
- Supporting all three arches of the feet: the medial longitudinal, lateral longitudinal and anterior transverse.
- The arch height in these three arches should allow for standard motion while restricting excessive movements, like pronation.
A randomized controlled study published in the Archives of Physical Medicine and Rehabilitation in 2017 yielded noteworthy results.1 These studies tested the use of a three-arch functional foot orthotic as described above, which led to significant improvements: low–back pain was reduced by 34.5%, and functionality improved by 18.5% when the foot orthotics were used alone and by 32.3% when used in combination with chiropractic care.
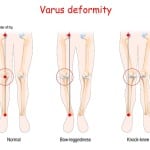
The knees: Understanding alignment for reduced strain
Since the surfaces of the distal femurs and proximal tibias are internally rotated at mid–stance, it becomes evident why the medial meniscus, anterior cruciate ligament and medial collateral ligaments often become involved in most knee conditions.
My professional experience has indicated the condyles of the knees typically display a rotational or posterior misalignment, also known as a subluxation pattern.
The hips: Enhancing mobility through correct alignment
As with the knees, the femur heads follow a predictable pattern with an internal rotation distortion. Motion palpation shows, in most low–back pain patients, restriction of external rotation in the femur heads. Hence, the correct adjustment or mobilization procedures can enhance joint mobility, contributing to improved overall motion in the hip joint.
The neurological aspect: Understanding joint dysfunction and pain
Joint fixation, misalignment or subluxation often leads to a complex dysfunction at the joint. In treating these complications, DCs focus on facilitating two main neurological aspects.
The first aspect derives from pain and symptomatology, which typically drives most patients to seek chiropractic help, and the second aspect is neurological.
The hypomobility, fixation or subluxation that occurs in any joint results in decreased firing rate of Type 1, 2 and 3 mechanoreceptors, which in turn increases the firing of Type 4 mechanoreceptors, also known as nociceptors.2
If the nociceptive impulses are intense enough to surpass the sensory cortex threshold, the pain sensation will be experienced. However, most nociceptive impulses fail to reach this threshold as pain thresholds are, by nature, relatively high.
What additional roles do nociceptors play? Nociceptors reflexively activate the sympathetic nervous system in a cumulative fashion, thereby triggering the “fight or flight” mechanism to some degree.3-5 This reaction incites shifts in physical parameters, such as heart rate, blood pressure, respiratory rate and even cortisol levels, a process identified as dysafferentation.4,5
It is important to note any degree of restricted range of motion in a joint will induce an increase in nociceptor firing. This response is cumulative as well.6,7
Deciphering the value in examining joints, whether symptomatic or not, is thus crucial. Particularly, the restricted range of motion, a significant indicator I’ve observed, merits attention, followed by the necessary adjustment. If the indicator changes, the doctor of chiropractic knows the procedure has an effect.
In essence, our patients typically arrive at our offices presenting a heightened state of tension and being more symptomatic, only to depart in a more relaxed state, displaying fewer symptoms.
Final thoughts
In conclusion and for reasons both structural and neurological, I firmly believe it’s integral to meticulously examine and appropriately adjust, support and rehabilitate the feet, knees, hips and spine in the active patient who presents with low–back pain and related lower extremity symptomatology.
MARK CHARETTE, DC, is a 1980 summa cum laude graduate of Palmer College of Chiropractic and a former all-American swimmer. A member of the Foot Levelers Speakers Bureau, he is a frequent guest speaker at chiropractic colleges and has taught more than 2,200 seminars worldwide on extremity adjusting, biomechanics and spinal adjusting techniques. He has authored a book on extremity adjusting and produced an instructional video series. His lively seminars emphasize a practical, hands-on approach.
References
- Cambron JA, et al. Shoe Orthotics for the Treatment of Chronic Low Back Pain: A Randomized Controlled Trial. Arch Phys Med Rehabil. 2017;98(9):1752–1762. PubMed. https://pubmed.ncbi.nlm.nih.gov/28465224/. Accessed Dec. 6, 2023.
- Guyton A. Basic Neuroscience. 2nd edition. Philadelphia: W.B. Saunders, 1991. Internet Archive. https://archive.org/details/basicneuroscienc00guyt/page/n3/mode/2up. Accessed Dec. 6, 2023.
- Hooshmand H. Chronic Pain: Reflex sympathetic dystrophy, prevention and management. Boca Raton, FL: CRS Press. 1993:33–35. Taylor and Francis. https://www.taylorfrancis.com/books/mono/10.1201/9781315139395/chronic-pain-hooshang-hooshmand. Accessed Dec. 6, 2023.
- Nansel D, Szlazak M. Somatic dysfunction and the phenomena of visceral disease simulation: a probable explanation for the apparent effectiveness of somatic therapy in patients presumed to be suffering from visceral disease. J Manip Physiol Ther. 1995:18:379–397. PubMed. https://pubmed.ncbi.nlm.nih.gov/7595111/. Accessed Dec. 6, 2023.
- Slosberg M. Effects of altered afferent articular input on sensation, proprioception, muscle tone, and sympathetic reflex responses. J Manip Physiol Ther. 1988:11:400-408. Pub Med. https://pubmed.ncbi.nlm.nih.gov/3069947/. Accessed Dec. 6, 2023.
- Kent C. A Four-Dimensional Model of Vertebral Subluxation. Dynamic Chiropractic. Jan. 2011. https://dynamicchiropractic.com/article/55080-a-four-dimensional-model-of-vertebral-subluxation. Accessed Dec. 6, 2023.
- Smith, HS. 2005. The Peripheral Muscarinic Dysafferentation (PMD) Theory. Published: Dec. 4, 2011. Albany Medical College, Albany, NY, US. Taylor and Francis. https://www.tandfonline.com/doi/abs/10.3109/J426v01n02_04. Accessed Dec. 6, 2023.